
Podcast: Play in new window | Embed
Subscribe: Apple Podcasts | RSS
Known as the “great imposter,” Lyme disease is a growing epidemic that can be difficult to diagnose as well as treat. While you might think that in order to get lyme disease, you needed to discover a bull’s eye rash somewhere on your body after taking a walk in the woods, that notion may no longer be true. It appears that more people with chronic poor health (especially with many autoimmune symptoms) are discovering that they too may have undiagnosed lyme disease that’s been left untreated for a long, long time.
I recall having a friend in grade school who contracted Lyme disease, but I honestly didn’t understand what the big deal was. Considering that Lyme disease is “the fifth most nationally notifiable disease“ according to the CDC, it’s a mystery why there isn’t more public education about how it’s contracted and treatment options out there.
Until recording this interview, I always got freaked out by ticks. Now I realize how incredibly serious they are and worry that we are dropping the ball to something that could be a major reason why people don’t feel well, especially when they just aren’t getting any better. This was pointed out in a webinar I hosted with Dr. Jill Carnahan where she mentioned that undiagnosed lyme disease is a big potential factor for those who have adrenal fatigue if they’ve taken all of the diet and lifestyle steps and still aren’t getting better.
YES, this podcast interview is long. It is filled with so much detailed information that I didn’t have the heart to cut it down to the typical 30-minute format because if it helps just one person, then I’m glad it’s all here.
I urge you to share this post with friends and family, especially those who have been diagnosed with lyme disease or even those who are incredibly sick and just can’t seem to get better. Perhaps this critical information will help them get back on the road to feeling better sooner.
CLICK HERE to listen and subscribe through iTunes!!!
Then take a moment and leave a review on iTunes sharing what you’ve learned and why others would benefit from subscribing as well!
Everything You Need to Know About Lyme Disease with Kevin Passero, ND

Jennifer: Welcome back to the Gluten Free School Podcast. I’m your host, Jennifer Fugo. Today, we are going to talk about Lyme disease.
I have a guest back with me. Actually he was a guest on one of my favorite podcasts. His name is Dr. Kevin Passero. He’s a licensed naturopathic doctor whose mission it is to bring cutting edge natural and holistic therapies to the Washington DC Metro area and to educate people on the value of naturopathic medicine across the country.
His practice focuses on an individualized approach to medicine with his goal to help people uncover the answers as to why their body is in distress and find the solutions necessary to restore optimal health.
Dr. Passero completed four years of post-graduate naturopathic medical education at the National College of Naturopathic Medicine in Portland, Oregon after receiving a Bachelor’s Degree in Environmental Biology from the University of Colorado. He is a former president of the Maryland Naturopathic Doctors Association and is an active member of the American Association of Naturopathic Physicians.
Welcome back to the podcast, Dr. Passero!
Dr. Passero: Thank you, Jennifer! Thanks for having me. I am glad you enjoyed my previous podcast so much.
Jennifer: I did! I learned so much about GERD and now you’ve got your own book out about that now. We can mention that at the end for sure.
But I feel like this issue of Lyme disease (I really appreciate, before we even get into anything) that you’re willing to sit down and talk to us all about this because I feel like so many people are now getting this diagnosis of Lyme disease. They just don’t even what it is.
I think of Lyme disease as being bitten by a tick. But maybe that’s not the correct association. Could you just describe to us a little bit about what exactly Lyme disease is?
Dr. Passero: Sure! Technically, Lyme disease is only a condition that you can get by being bitten by a tick. At this point, the only confirmed or known vector, which is the insect or animal that transmits the organism, the spirochete, which is the bacteria, the Lyme disease bacteria is a tick.
But it’s a very confusing picture because Lyme disease as we have seen and we’re starting to learn can present in many, many different ways and there seems to be a lot of confusion amongst healthcare professionals spanning from naturopaths to medical doctors to infectious disease specialists to nutritionists and all across the board as to what constitutes a case of Lyme disease. I think that’s one of the most important things that people have to start to understand.
There is the acute, most obvious presentation of Lyme disease. Somebody gets bit by a tick. They see where the tick bit them. They remove it.
They may be present with the classic bull’s eye rash, which is this very, very unique reaction that occurs in Lyme disease. It is unique only to Lyme disease. A bull’s eye rash is considered pathognomonic for Lyme disease, meaning that a doctor doesn’t have to do any further testing to confirm a Lyme disease diagnosis if that particular rash is present. So it’s very unique to it. And then maybe they present with fever and joint pains and that’s a very classic acute onset Lyme disease.
Where it gets very confusing, Jennifer, is that many people obviously struggle with various aspects of their health and they’ve had ongoing health struggles for a long period of time and many times, they go into doctors’ offices and they haven’t been given any answers as to why they feel so sick. It may be fatigue. It may be joint pains or body aches.
Lyme disease testing, as we’ll talk about in the show, can be a bit controversial and not as black and white as many other tests. There are many clinicians out there that are looking at these cases of people that are chronically unwell despite what looks like very good treatment from conventional medical doctors and specialties. They’re still very unwell.
Well, we’re starting to wonder, “Is it possible that infections are a component to their case and one of the underlying reasons why they are feeling ill?” because it’s typically something that has never been addressed? That’s what starts leading us down this very muddy road, new avenue of chronic Lyme disease. Does it exist? Does it not exist? How do you test for it? How do you treat it?
Basically, that’s where I think many of your listeners might be falling into the category of they’ve been unwell or struggling for a while and they’re now getting diagnosed or they’re hearing about Lyme disease and it’s starting to bring up a lot of questions.
Jennifer: Is it possible that you could have been bit by a tick and not even realize it and you end up with Lyme disease?
Dr. Passero: Yes, right. So first of all, tick bites don’t cause pain. Unlike a horsefly bite or other animals that bite, sometimes they itch and sometimes they hurt. With ticks, you feel nothing. There’s really no way to know just based on the sensation whether or not you’ve been bitten.
Number two, Lyme disease is most likely to be transmitted at certain times a year by certain types of ticks. Usually, it’s the juvenile ticks, the very, very baby ones, which come out in the springtime.
That’s because they basically haven’t really had their first meal. The Lyme disease organism can be transmitted to them basically from the mother who’s spawning them. And when they’re out looking for their first meal, they’re very aggressively looking for hosts to feed on.
And in addition, they are tiny, sometimes smaller than a sesame seed and sometimes no larger than the head of a pin. They’re tiny, tiny little insects.
It’s very possible that one could attach, could feed. You never felt it, you never noticed it. It dropped off, it went on its merry way and you never remembered actually having a tick bite, nor seeing a tick bite. And not everybody that gets bitten by a tick or gets Lyme disease has that pathognomonic rash – bull’s eye rash. This only happens in a percentage of people that get bitten by tick or that contract Lyme disease. So you may never have had a rash. You never may have seen the tick, you have never felt the tick, but you may have had some of these Lyme spirochetal organisms transmitted into your body.
And they have a very, very slow growth cycle. Sometimes, it may take years before their population grows enough to even cause the first set of symptoms.
Jennifer: What would those symptoms be? If we’ve got people who’s listening to this and they’ve just not felt well for a really long time and they’re trying to put pieces together, but nothing really makes sense maybe – and I know that some people say, “Maybe I have Lyme disease.” It always seems to get thrown out there. So what would be some key signs and symptoms that people would look for?
Dr. Passero: Yeah. It’s probably a really tough question. It’s almost impossible to answer because Lyme disease is often called the great imitator. It’s a relative of syphilis. Syphilis is another type of spirochetal organism that is basically the cousin of the Lyme organism.
And syphilis was even called the great imitator, meaning most any condition that you have could possibly be related to Lyme. That’s one of the problems.
There are two sides of the fence. You have a very conservative group of very conservative position from the CDC and from the Infectious Disease Society of America, of those doctors where there’s a very set criteria of symptoms and testing that has to be in place.
And then there is this whole other side of it – MDs that have looked at chronic Lyme, naturopaths, nutritionists, acupuncturists where you can almost look at any case and potentially call it Lyme. So you’ve got to have somewhere in between.
But some of the primary symptoms in the early phases, you may have a fever and you may have joint pain, headaches, stiff necks, pain and swelling in the large joints. The knees seem to be particularly repositories for the Lyme organism, so knee-swelling. There are shooting pains, which are very vague, heart palpitations, dizziness, visual changes, eye pain.
You can have autoimmune type conditions crop up. Fatigue is certainly a big component of a lot of Lyme disease. There’s brain fog and difficulty thinking, confusion, even neurological symptoms, numbness and tingling.
These are just for Lyme disease. There are many other infections that tick carry that are considered co-infections meaning that they’re commonly transmitted at the same time that a Lyme organism is transmitted and these are other things like Babesia, which is a parasitic infection that behaves very much like malaria where you can oftentimes see night sweat (it’s a very common symptom), daytime fevers.
There’s another organism called Bartonella, which is very commonly transmitted, which can cause some other hallmark symptoms like skin changes, odd stretch marks, pain on the bottom of the feet, high levels of anxiety.
The list goes on and on. We could spend the 40 minutes literally reading through a list of symptoms, but I suppose those are some of the top ones.
Jennifer: If someone gets bit, if they believe that they got bit by a tick or maybe you find a tick crawling on you – this happened to my husband a couple of weeks ago. We were sitting on the couch and all of a sudden, I saw something crawling up his shirt. And he said, “Oh my goodness, it’s a tick.” We weren’t even near the woods, but somehow he had a tick on him. And I’ve gotten a tick on me in the middle of a mall. It happens. Should you be concerned if you find a tick on your clothes that maybe you got bit by it?
 Dr. Passero: It’s a good question. It’s possible. I mean, typically, if you see one crawling on you, there’s no evidence that it’s embedded. The problem is when it’s embedded and it looks like it is feeding. That’s the only way it can transmit any of these nasty bugs, if it’s actually embedded in your skin.
Dr. Passero: It’s a good question. It’s possible. I mean, typically, if you see one crawling on you, there’s no evidence that it’s embedded. The problem is when it’s embedded and it looks like it is feeding. That’s the only way it can transmit any of these nasty bugs, if it’s actually embedded in your skin.
Typically if it’s crawling around, it’s usually looking for a place to embed. And usually if it’s crawling around, the first thing that you should ask is retrace your steps. Where was I? Find out. “It was at the mall. But did I walk through? Did I take a shortcut through a grassy area or through some woods or anywhere where I may have just picked this thing up?”
Yes, your husband is sitting at home on the couch, but was he out mowing the lawn before? Or perhaps do you guys have a pet or an animal that could have maybe brought the tick in?
If it’s crawling on you, I think your best assumption is probably that it hasn’t bitten you yet. Sometimes, you can also tell by the size. Typically, when a tick has fed for a while, it becomes really large and engorged. It almost looks like a swollen blister because it’s full of – it is gross, but it’s full of its blood meal.
So if it’s not full of its blood meal, it doesn’t look engorged, you can pretty safely assume that it hasn’t just stopped feeding and it’s trying to crawl off of you to find a way off. But really, what you need to be worried about is when you find the tick embedded in the skin or you have an area or a site that looks suspicious like it might have been a tick bite.
I would say as well that one of the other biggest misconceptions is that people get bit by a tick and a lot of times, they do get a rash. When they go online or they go to their doctor, it doesn’t look like this very characteristic bull’s eye rash, but it is a very suspicious looking rash.
So anytime that there is a rash of more than a few circular rashes that’s larger in diameter, maybe one to two inches, I would highly suspect the possibility of Lyme disease even if it’s not a bull’s eye rash.
And if it’s a large rash more than three or five inches in diameter and it doesn’t have bull’s eye characteristics, you can still have what looks like what is a pretty much classic Lyme disease rash that doesn’t have the bull’s eye characteristics.
If you have a tick bite and there’s any real suspicious looking rash, you should definitely have it looked at. A lot of times, the immune system will respond to just the tick’s saliva and some of the other things that the tick puts into. So it’s normal, a lot of times, to have a little bit of redness around the bite mark, even lasting maybe one to two weeks. But if it’s a larger area that looks really suspicious, this is something that absolutely needs to get looked at and I think would probably require some treatment.
Jennifer: There are very practical questions here because I honestly don’t know the answers. I want to know and I’m sure other listeners would probably want to know this.
Dr. Passero: Sure.
Jennifer: If you get bit by a tick (and you say it’s embedded), do you pull it out or do you need to go to the doctors to have them remove it?
Dr. Passero: No. You can pull it out yourself. There are methods for doing it. Number one thing, all of the old wives’ tales – there are so many different things. Smother it in Vaseline. Burn it. These are all bad ideas.
Jennifer: Don’t do those.
Dr. Passero: You don’t want to do any of those things. No. First of all, coating it in Vaseline, the idea is that it cuts off and the tick can’t breathe and it will back itself off. There’s no evidence at all that that is necessary.
Ticks really don’t need much oxygen and Vaseline just basically makes it slippery and when you do have to pull it out, it makes you have to squeeze it more. It makes the tweezers slide. And basically you want to avoid things that basically cause the tick to put things back in your body. So over-squeezing it and over-manipulating it can be problematic.
Unless it’s an area that you can’t reach, you really don’t need a doctor. There are a few techniques to do it. You want to grab it as close to the head as possible and you want to pull it straight up and back a little bit, meaning almost tilting the tick on its back, just very slightly and pulling up gently.
One of the best tools that I’ve ever seen for this was demonstrated to me at a Lyme disease international conference that I was at. It is called the “Tick Twister.” It was developed by a company I believe in Germany or Switzerland. The tick’s area where it embeds is barbed. It’s a like a fish hook that’s barbed. So it’s very difficult to pull it straight out.
If the tick’s head gets left in your skin, the head and the saliva glands where the Lyme disease organisms and these other nasty organisms live, it can continue and you’re at risk for transmission as long as the head is still in you. Plus, if the head stays in, it also creates an opportunity for infection, just general infection.
The Tick Twister, because the mouth of the tick is barbed, it actually takes the tick and it grabs it in a certain way and it twists it. And if you were to take something barbed and put it in a piece of Styrofoam, if you try and pull it out, it will pull the whole block of Styrofoam right up with it. If you slowly twist and lift, it comes right out without even moving the block of Styrofoam.
So it’s this ingenious way of looking at the mechanics of the tick and the anatomy and basically ensuring that we get the best removal because you do want to try and get the entire tick out with the head without overly squeezing it or manipulating it.
Burning it doesn’t work at all. None of those things work. You can burn it once you remove it although I wouldn’t recommend that either. But those are the best options for removal.
Jennifer: And if it happens that your pet, say a dog or a cat, goes outside and you live in a woody area, can they get bit and carry Lyme disease as well?
Dr. Passero: Absolutely! Animals get very ill with Lyme disease, particularly dogs. Horses are very susceptible. I haven’t heard as many cases with cats, but maybe that’s just because I don’t know as many cat owners as I do dog owners. But it can transmit. Cats are a huge repository for that other co-infection called Bartonella.
But yeah, dogs can have it and they can get sick with it with the same symptoms as humans. We don’t really measure brain fog in a dog, but you can see fatigue and lethargy. And certainly, the most common is arthritis and arthritic changes in dogs. Dogs can be pretty sick with it.
And then your dogs can also carry the ticks in. They go out in the wooded area and they do their business. They chase a squirrel and they pick up the tick, they bring it inside. The dog sleeps in the bed. You guys are sleeping. The tick crawls off the dog and crawls on to the person.
I have had this happened personally when I had a dog. It used to sleep in my bed. I wake up in the morning and I have ticks embedded in me. It came from the dog.
So those are all possibilities. I try and get people to get their animals out of their bed.
Jennifer: How common is Lyme disease? I often think that it is something we should all be aware of at least in the US, but I’m not even sure with certain regions. Perhaps you know if this is just an issue in the US or North America or if this is something that is more worldwide of a concern. How frequent, if you know those statistics, does Lyme disease show up?
Dr. Passero: It’s very common. It is the most commonly reported vector-borne illness in the United States meaning it’s the most common disease of something that’s transmitted by an insect.
Basically, they report about 30,000 cases of Lyme disease to the CDC every year. But there was an analysis that was done where that was just considered the tip of the iceberg where really a new estimate, according to the CDC, was more than 300,000 Americans are diagnosed with tick-borne diseases each year. That has to do with reporting and poor ability to get good diagnostics and a true understanding of the condition and disease and how to diagnose and report it.
It is 10 times more common. That’s even from the CDC. If those are the CDC estimates, a lot of times, the true estimates are even greater than that.
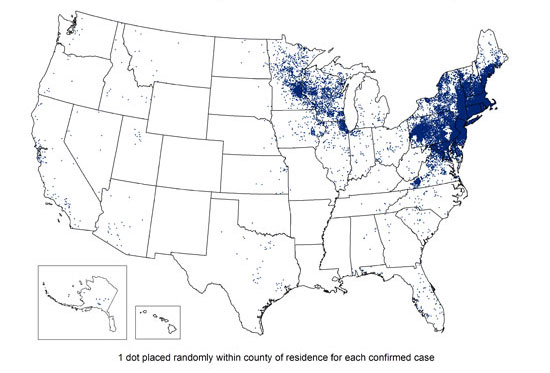
Confirmed cases of lyme disease as of 2013. (Image from the CDC.gov -http://www.cdc.gov/lyme/stats/maps/map2013.html)
It is a very big issue in the United States. Every state in the United States has Lyme disease. There isn’t a single one that doesn’t. There are areas that are more common. There are certain states where it’s considered endemic, meaning that it has the highest rates and that the organism is considered to be at high rates in all areas of that state. Where I live, Maryland happens to be one of them. Minnesota is another one and New York, Connecticut. Some of the other states on the East Coast are one of them.
So the East Coast in Lyme, Connecticut is where the first case of Lyme disease was reported, which is where it got its name. So it’s obviously spread out from that area. The Northeast Corridor, stretching all the way down to East Coast and into the Southeast has very high rates of Lyme disease.
You also do see high rates on the West Coast, even in California, Oregon, Washington State, even in the Midwest. I said Minnesota is an endemic state, one of the highest rates of Lyme disease. Pretty much there isn’t a state that doesn’t have it.
And the condition does go worldwide. It is present in very high numbers in Europe, even in areas like Africa. Pretty much every continent is dealing with Lyme disease to some degree or another.
Jennifer: Wow. I had no idea. I honestly thought maybe it was just North America. I did not realize that you actually have to be concerned about this.
I’m sure that everyone listening to this is going, “What does this have to do with gluten?” We talk a lot about gluten. You and I talked about GERD and gluten, what the connection was.
Why do you think that people who see functional medicine doctors or naturopaths like yourself because they aren’t getting straight answers. And Lyme disease ends up being suspected or found. Why do you think that all these people are not getting help in the conventional medical system? It just seems like Lyme disease is a big issue.
Dr. Passero: Sure. The classic scenario is that someone presents with a subset of symptoms. Maybe they’re having joint pains or shooting muscular pains like we talked about or they’re experiencing vertigo or dizziness or headaches or some type of chronic condition.
They see their primary doctor. Their primary doctor runs some blood test, tries some initial therapies. Blood test seemed normal. Initial therapies are failing. They maybe send him to a specialist. “Okay, you’ve got all these pain issues. Your blood test looked pretty normal. It’s not responding to my recommendation to take Advil or whatever it is. Why don’t you see a rheumatologist?”
The patient goes to a rheumatologist. They get a full slew of work up from the rheumatologist. Maybe there are one or two markers that are abnormal, but not enough to categorize them with a rheumatological disease like lupus or rheumatoid arthritis or something along those lines. The rheumatologist is scratching their head, going, “Well, it looks like this, but your labs don’t really match it. Maybe we can try this medication and we’ll put you on Lyrica or some other type of med.”
Patient either says, “I’m not comfortable with that looseness of the diagnosis to try the medication. I’d rather only reserve medications when I actually know exactly what the diagnosis is.” That may lead them down a different road. Another patient may try the medication recommended by the rheumatologist and oftentimes because it’s not treating the actual issue, they actually don’t get any results from it.
So they’re still feeling pain. They’re still having dizziness or vertigo or whatever their subset of symptoms is. And they go to a different rheumatologist or the rheumatologist sends them to a neurologist and they go through that whole battering of workups. And they’ve been pretty much through every possible workup specialty and potential treatment from everything that Western medicine has to offer and they’re still left sick and unwell and wondering what in the world is going on with their body.
And then they oftentimes end up in the office of a functional medicine doctor who sits down and takes a bit of a different approach and says, “Well, why isn’t your pain responding to the treatments that should work for a rheumatological type of condition or this type of condition or that type of condition? Maybe something else is going on.” A lot of times, because Lyme is the great imitator and can cause a lot of symptoms, more doctors are becoming aware that an undiagnosed infection from something like Lyme disease may be a very causative or primary factor in why these people are still ill.
For people who practice functional medicine or naturopathic medicine, which is basically the same thing. It’s looking for the root cause of an illness, except naturopathic medicine is much older than functional medicine. The idea is to look for the root cause and to find out why. And if you ask that question enough times and you really want to try and get to the answer of why is this person sick, you have to start going down these different roads. Infection, we’re finding, is a road that needs to be explored these days.
Jennifer: If you get Lyme disease, I’m wondering if you can get rid of it. Is this a chronic issue if you get that diagnosis that you’re going to have Lyme or you’ll be dealing with Lyme for the rest of your life?
Dr. Passero: It depends on the case and it depends on how it’s treated. And it depends on the person. Some people, unfortunately the answer is yes. For many people, the answer might be no.
What we don’t really understand, especially in people with chronic Lyme, is it a result of the fact that there are still bacteria left that are causing problems? Or is it a result of the fact that maybe – we know Lyme disease increases risk factors for autoimmune conditions. Is it possible that even the infection may be gone, but there’s some autoimmune activation that has happened that’s contributing to inflammation and problems?
Lyme organisms cause so many symptoms because they release toxins. Most bacteria do. Another possibility is that some of the toxins, which are highly fat-soluble, get stuck in the body. And even if the infection is gone, you’re still dealing with a high burden of toxins that continually circulate in the body that makes it difficult to feel well.
These are all working theories. Sometimes you can look at these working theories and apply certain therapies and take somebody who – I’ve worked with these patients – has had three years of continuous intravenous antibiotic administration, who probably has killed off most of the organisms, but is still dealing with a fair amount of symptoms. Give them certain therapies that work to detoxify the toxins out of their system. And all of a sudden, they start to feel better. Or you work on things that modulate immune function and they start to feel better.
And then for some people, it’s very straightforward. They get bull’s eye rash. They get some arthritic changes. They catch it early. They see a doctor who has a good heads up. It’s treated appropriately for long enough. It goes away and they’re done. They never have another symptom for the rest of their life.
It’s not, in my opinion, about do you always have Lyme disease because it’s very likely that probably a large percentage of the population has some type of or one or a few Lyme organisms may be in their system. It’s more a question of how your body’s balancing and living in equilibrium with that organism.
So it’s a very difficult knot. It’s like everything else is with Lyme. It’s not an easy question to answer.
Jennifer: Yeah. I guess you have to really approach each patient from a very individualized space. Otherwise, the treatment is probably not going to work because like you said, there are so many different factors here.
Dr. Passero: Yeah. I mean most of the basic concepts around treatment are the same. I mean you always start typically with killing the organisms. That may come from antibiotic therapy, which can be effective. Or many people choose to use herbal or botanical therapies, which also can be very effective.
Jennifer: It’s interesting because antibiotics – my audience is no stranger to antibiotics and also the amount of devastation that antibiotics can do to the gut flora. So I guess the question is if you find out that you have Lyme disease, say you really don’t want to go the antibiotic route, what are some things that they can maybe do some research on and present to their doctor that are not antibiotics?
Dr. Passero: Sure. Again, I think it really depends on the case because certainly in the right circumstances, I think antibiotics can be an incredibly valuable tool. And in many circumstances, especially if something is caught early, I actually recommend and oftentimes prescribe antibiotic therapy. I do that typically in conjunction with other therapies, but antibiotics can serve as a very good primary treatment for these issues.
Some people who are very sick, Jennifer, who are presenting with very severe symptoms, neurological symptoms, losing function of some of their limbs, they’re having major neurological problems, major visual changes, Bell’s palsy, very difficult problems, a lot of times, you need some antibiotics to come in to just stabilize that case and get the infection under control at the beginning where I don’t think that’s oftentimes enough in the long run. But in the beginning, it oftentimes is a good start.
For some people, you need to really work with somebody that understands the different options and can help you understand the different options so that you can make a good clinical decision. I think the part where it becomes really confusing is a lot of people who have been sick for a long time or are just getting diagnosed with chronic Lyme, many of the treatment protocols for treating chronic Lyme do include extended courses of multiple antibiotics. Some people might be horrified to hear this, but it oftentimes includes three to four antibiotics given simultaneously for typically anywhere from 12 to 48 months.
Jennifer: Oh, my goodness!
Dr. Passero: Right? So a lot of times, that’s the reaction. That is probably the gold standard treatment for doctors that have been exclusively dealing with chronic Lyme, which is a condition that is not yet recognized by the more traditional Infectious Disease Society guidelines and the CDC don’t really recognize chronic Lyme disease. But many of these people who have been sick for a long time, when you get them on these antibiotic protocols, a lot of times they do start to get well.
Obviously, it takes a very hard toll on the body to use that many antibiotics. And I’ve seen people on those antibiotic therapies for three to five years.
Jennifer: Oh, my goodness.
Dr. Passero: So it does get tricky and it does beg the question – what else can we do from a non-antibiotic standpoint because of the tolls that it takes on the body and other ways to get the infection under control? There are many herbal protocols that have been very helpful.
Dr. Lee Cowden, a cardiologist from Texas who’s got very much into functional medicine. He started just from patients that were walking in his door, getting introduced to Lyme disease. And he ended up developing a very successful herbal protocol called the Cowden Protocol.
It’s somewhat expensive. It’s very labor-intensive because you have to take doses of these different herbs about four times a day. And you take them for a minimum of typically nine months up to a year, sometimes even longer.
But it is not antibiotic-based and it can have very, very good clinical outcomes. Some say and some small clinical office trials with about 2000 patients, it got about the same benefit as using these really aggressive antibiotic therapies, but it’s obviously not antibiotic-based. But only people who can afford it and are willing to go through the process of taking all those herbs at different times would be good candidates.
There’s another fantastic herbalist. His name is Stephen Buhner. And he wrote a book called Healing Lyme Disease Naturally. He has some very good protocols that I’ve seen many patients and other people that I’ve met in the Lyme community do very well on.
There’s a myriad of many other companies that a good clinician who’s working with these issues should know about that can be very effective. And there are some other really interesting therapies that are coming to light that fall under the category of oxidation, which uses ozone therapies. That can be ozone delivered rectally or intravenously, mixed with the blood. And using hydrogen peroxide therapies delivered in various fashions that are also showing a lot of promise when it comes to treat infections without the use of antibiotics.
Jennifer: If someone is uncomfortable with or perhaps they’ve tried the antibiotics, has it ever happened where someone tried the antibiotics and they didn’t work and maybe now they want to move on to something else that is non-antibiotic-based?
Dr. Passero: Yes, it’s very common that that happens. Or somebody may go through a year of antibiotic therapy and improve and then to find that a year later, the symptoms are starting to return and they are looking for a different option besides the antibiotic therapy to get it under control. This might be someplace they would turn.
Many people when they’re diagnosed at the outset – this is a decision that I make with people all the time because I’m often one of those functional medicine clinicians, with appropriate testing and building appropriate enough case around the diagnosis, will say, “I really suspect that you have an infection and I suspect that that infection is Lyme disease or possibly other co-infections are related to it. And I think that some of the chronic symptoms you’re experiencing are very much related to it.” And of course, the next question out of their mouth is “How do I get rid of it?”
And then we have a discussion about here are the options that are on the table. We can treat it this way or that way. And I help patients make that choice if they don’t already have a strong feeling about it based on their case and how they’re presenting the severity of their illness and those types of factors.
Jennifer: So I think the takeaway message that I’m getting from all of these is really that – I know that everything serves a place. Antibiotics, there’s a purpose for them. I think we’re so used to them being overused, but in this instance, it is something that you might not want to just discount immediately. You should really work with someone that knows all the options and can help you make a decision that’s going to be best for your long term care.
Does that sound about what you’re saying?
Dr. Passero: Yes. Every case needs to be weighed individually. While using multiple antibiotics for long periods of times comes with risks, in some cases the benefit outweighs that risk and in some cases, it doesn’t. In some cases, people aren’t just giving the option.
I would say the biggest problems around Lyme disease are the testing. That’s why most things get missed because we don’t have the greatest testing and most of the conventional tests for Lyme disease miss I would say a majority of the diagnosis. So these people are never even told that this might be an issue and they’re never given any treatment options.
And then the second issue is just trying to navigate around what is the best form of treatment and getting treated for an appropriate amount of time with the right therapies.
Jennifer: Are there any tests that you run that would be different from perhaps a conventional doctor?
Dr. Passero: Yes, there are. There are many different tests because you can’t just use the standard lab tests that are typically done from – you can and sometimes they do catch the cases, but a lot of times, they miss it. There are certain labs that have developed more sensitive, more specialized testing to help clinicians like myself who suspect that Lyme disease may be an issue and who aren’t 100% wholly confident in the standard tests that are given.
We need to build the case for diagnosis around this patient because we just don’t want to start giving people antibiotics or complicated herbal protocols based on nothing. We usually need some type of objective finding to confirm our clinical suspicion.
IGeneX in California is one that’s been around for a long time with the good name in testing for Lyme disease. There’s a lab called Fry Labs in Arizona. There are labs all over the country that have developed more specialized techniques for helping doctors sort through this issue.
Jennifer: Okay. So you’re not left with just the test that you’ll get at a conventional doctor’s office.
Dr. Passero: You are if that’s the only doctor you see.
Jennifer: Fair enough. Fair enough. So I appreciate that you’re willing to talk about this because I know that you see patients like this a lot. This is your wheelhouse. This is something that you deal with it sounds like quite regularly as far as patients are concerned, especially concerning that Maryland where you live is a hot spot for this issue.
I definitely want to encourage everybody to go check out your website and contact you if they believe that they have any questions around this. And you do see and consult with patients throughout the United States? Or is it worldwide you can consult with patients if they have questions with Lyme disease?
Dr. Passero: Yeah. The Internet has basically shrunken our world. My ability to treat and the options and things I’ll have to treat people vary based on whether or not I can see them in person or not. I mean I can certainly consult and help educate or guide people to appropriate resources if they’re not able to actually see me.
Jennifer: Very cool. And you have a great book. I know it’s slightly off topic. And we talk a lot about GERD and acid reflux. But I just want to remind everyone that it’s an excellent book. It’s called Drug-Free Acid Reflux Solution, which is available on Amazon as well as your website. Correct?
Dr. Passero: Yeah. It’s not oftentimes as exciting an issue as Lyme disease, but it’s something that many, many people suffer from. We’ve sold thousands of copies of the book. The feedback has just been fantastic.
It’s not the fanciest book. It’s my first book. It has a nice little soft cover. It’s not overly expensive. And at the end of the day, the feedback we’ve been getting from people who have purchased it is that it is working beautifully. Gratefully, it doesn’t surprise me because the entire book is based on my 10 years of clinical practice in dealing specifically with GERDs. So I was just applying in the book or writing in the book what I saw work in my practice. It seems to be working beautifully.
Jennifer: That’s really great when you get feedback about your book and that people are actually benefited from the material that you’ve put out there.
Dr. Passero: It’s very gratifying. Yes.
Jennifer: I know. Tell everybody about your website so that they’ll be able to visit you.
Dr. Passero: Sure. The website is www.GreenHealingNow.com. There are lots of blogs and things listed on there.
The issue of Lyme disease is a bit controversial and is a very sticky issue. So I don’t really have a lot of information on my website about Lyme disease. I try and keep the website just more general informational, but if people have specific questions about it, they’re more than welcome to send an e-mail or contact the office and speak with myself or myself.
Jennifer: Wonderful. Thank you so much for joining us. I really appreciate it, Dr. Passero.
Dr. Passero: You’re welcome, Jennifer! It’s always a pleasure. Thank you for having me on.
Jennifer: Absolutely. Everybody, please stay in touch with Dr. Passero. If you haven’t done so yet, I highly encourage you to check out his other podcast interview. It was again a real eye-opener for me all about GERD and heart burn and all these chronic conditions that they nag at you.
And if you have been diagnosed with Lyme disease or you suspect that you have it, leave a comment below this podcast and let us know what your experience has been. It would be wonderful to hear from everybody because having a community where you can actually share what’s going on or what your experience has been is a really great way to connect and also empower others in our community to take that step to get better.
Our health is our own journey and we’re also the best advocates for our own health. And by sharing, it really does make a big, big difference.
Thank you so much for joining us today. I really appreciate it. If you haven’t yet, subscribe, rate and review the Gluten Free School Podcast. Hey, I’ll see you again next time. I really appreciate all of you sharing and listening and tuning in. Thank you so much and have a wonderful day!
The links referred to in this episode are:
Dr. Kevin Passero – http://www.GreenHealingNow.com
Facebook: https://www.facebook.com/GreenHealingWellness
Twitter: http://www.twitter.com/drpassero








Enjoyed this podcast very much. Will share my symptoms. I have been bitten twice by ticks. Once 2007 and it was infected for a time, finally healed up. I did not get any symptoms then. I had a bullseye reaction in 2013 to a tick bite and did a round of Doxycycline beginning at the ER. It did itch as well, because I am very sensitive to bug bites in general. I was given 2 Benedryl & recovered. 2014 I began having breaking out on one area of my back, felt like bugs crawling under my skin, although 2 different Dr.s did not think too much about it as a problem. I periodically have this in the spring and end of summer. New symptom this year, dizzy and felt faint, but didn’t pass out, shook a lot and my feet and hands became cold, my head felt feverish and felt flushed, heart palpitations.This passed within a few minutes and was ok. Second time went to ER, Dr. said probably I had a virus in my inner ear. Well this passed after a whole day. I also have digestive issues. Seriously thinking of getting tested. Thanks again Jennifer and Dr. Passero! Diane Whitlock
Thanks so much, Jennifer and Dr. Passero, for an excellent podcast. Such an important and timely topic! I have chronic Lyme, just diagnosed early 2015 after 30 years of intermittent and increasing health issues. I’ve had to look far and wide for answers and am so glad I didn’t give up. My story is very typical, just as you describe here. I’ve done a multitude of constant natural therapies for 30 years ,thinking it was ‘just’ adrenal fatigue’, thyroid issues, chronic fatigue, food sensitivities, leaky gut , etc., but could still not regain my health. Now I am on a ‘cocktail’ of 3 antibiotics prescribed from a Lyme Literate MD. Thanks so much, Dr. Passero, for your considerable knowledge, open attitude and for raising public awareness.
I got 2 tick bites in June. They were like really itchy mosquito bites that didn’t go away. After about 10 days, I realized that they changed and looked like bullseyes and got treatment with antibiotics right away. Just an fyi of how they can feel. I didn’t feel getting the bites, but they were definitely itchy from the beginning.
I’ve struggled with Lyme, coinfections, & MARCoNS. I was bit 3-4 years ago and thought (no real knowledge of Lyme) that if I didn’t have symptoms or a bullseye rash I was ok. About 2 years ago I started having symptoms I thought were Hashimoto’s thyroiditis troubles. I found that my PCP & endocrinologist were not figuring it out, so I found (through a FB thyroid support site) an integrative doctor who listened to my symptoms. He started treating me for my Hashimoto’s, but I wasn’t getting better. He suggested I be tested for Lyme. My results were equivocal. Long story shorter, I ended up with a LLMD doc who has put me on a mix of antibiotics, herbal drops, & key supplements. I’ve had to be gluten free, sugar free, & dairy free. I’ve learned that detoxing is huge with Lyme, I’ve also learned who my friends truly are. I have been mostly housebound, & it has been a difficult summer. But I’ve also learned to be grateful for what I do have. It’s a difficult road and I feel different every day.
People need to understand this bacterial infection is serious. Lyme is not publicized as much as cancer, and there are now more people with Lyme disease than cancer! It’s maddening to us Lymies! Better tests are needed as well as doctors who understand how to treat it.